Poor Quality Malaria Medicines: Using SBCC to Empower Instead of Create Fear
The Problem: Poor Quality Malaria Medicine
The malaria community has made great strides in malaria case management, including improvements in prompt care-seeking, testing with rapid diagnostic tests (RDTs) and treating with artemisinin-based combination therapies (ACTs) – contributing to a 37 percent global reduction in malaria incidence and 60 percent global reduction in malaria mortality between 2000 and 2015. However, recent studies have found several instances of poor quality malaria medicine in sub-Saharan Africa and southeast Asia that could threaten this progress because they do not contain enough of the active ingredient to treat malaria.
These poor quality medicines – due to issues with manufacturing, storage or theft – also create public health challenges 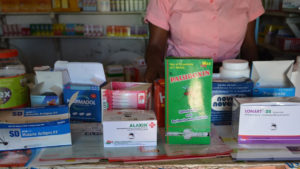 because they can negatively influence consumer behavior, waste individual income and national budgets, and contribute to artemisinin resistance. Adding to this problem is the fact that poor quality medicines are incredibly difficult to identify, because of how advanced counterfeiters have become and because nothing visually indicates when a medicine has been altered.
because they can negatively influence consumer behavior, waste individual income and national budgets, and contribute to artemisinin resistance. Adding to this problem is the fact that poor quality medicines are incredibly difficult to identify, because of how advanced counterfeiters have become and because nothing visually indicates when a medicine has been altered.
While activities aimed at improving international and national medicine manufacturing, procurement, regulation and enforcement can greatly reduce the burden of substandard, spurious, falsely labelled, falsified and counterfeit (SSFFC) antimalarials in the long run, they cannot eliminate the problem entirely, or protect today’s malaria medicine consumers from the dangers of poor quality medicines.
As public health professionals, it can be tempting to want to grab a megaphone and shout the news to whoever will listen, but it is important to consider the impact of our words on the populations we serve. For example, imagine you’re a mother living in a peri-urban area in sub-Saharan Africa. Your child has a fever and you suspect it may be malaria. If all you’ve heard for the past month are messages about the widespread prevalence of poor quality malaria medicine in your area, you may be less inclined to go to the formal health center to get your child tested and treated (if the RDT comes back positive) – you may instead turn to a traditional healer, witch doctor or community/religious leader. You may also opt to self-treat with medicine from an illegal hawker, because you are unaware or disinterested in the fact that the pharmacy at the health center has quality-assured malaria medicine (that would be prescribed based on the specific dose your child requires).
The Solution: SBCC and Non-Traditional Partnerships
While consumers and vendors cannot eliminate the presence of SSFFC malaria medicine in their area, they are in the position to decrease their risk by practicing positive buying, selling and reporting behaviors. Social and behavior change communication (SBCC) and advocacy can help raise awareness among key audiences and promote steps that can be taken to protect consumers, families and communities. Because of the complexity of this issue, identifying the best target audiences and messages often requires a comprehensive analysis of the malaria medicine situation and partnering with non-traditional partners that may not have a background in SBCC, such as supply chain specialists, regulatory agents, law enforcement officers or informal medicine vendors.
 The Health Communication Capacity Collaborative’s (HC3) collaboration with the Nigerian National Malaria Elimination Program and National Agency for Food and Drug Administration and Control (NAFDAC) in Akwa Ibom State, Nigeria shows the power of this approach. By following the P-Process, the team created and implemented a four-month campaign that targeted consumers who buy malaria medicines as their primary audience, and informal medicine vendors as their secondary audience.
The Health Communication Capacity Collaborative’s (HC3) collaboration with the Nigerian National Malaria Elimination Program and National Agency for Food and Drug Administration and Control (NAFDAC) in Akwa Ibom State, Nigeria shows the power of this approach. By following the P-Process, the team created and implemented a four-month campaign that targeted consumers who buy malaria medicines as their primary audience, and informal medicine vendors as their secondary audience.
The resulting TV and radio spots, posters, stickers and community volunteer materials focused on the presence of good quality medicine and the steps people can take (e.g. buy from licensed wholesalers and pharmacies, check for NAFDAC and expiration date on the ACT pack, verify medicine by texting the code under the scratch pad to the Mobile Authentication Service). An end-line evaluation found that after this short, concentrated campaign, Akwa Ibom residents not only reported improvements in knowledge, but the majority of those exposed to the campaign reported that they would do something differently the next time they needed antimalarial medicine.
Want To Learn More?
Building program managers’ capacity to develop and implement SBCC strategies to address issues of poor quality malaria medicine is a priority for HC3’s Malaria team. This week, HC3 is hosting a webinar and launching an online implementation kit (I-Kit) on the topic. The webinar will take place on Wednesday, November 2, 2016, at 9 AM ET and will involve presentations from a range of stakeholders working on this issue, including presentations from:
- Martin Cinnamond (Team Leader, The Global Fund to Fight AIDS, Tuberculosis and Malaria), who will discuss what the Global Fund has been doing with respect to poor quality medicines.
- Jennifer Wray (Senior Malaria Advisor/Commodities – USAID/President’s Malaria Initiative), who will discuss techniques and findings of quality assurance tests.
- Cori Fordham (Program Officer, HC3), who will introduce HC3’s new online implementation kit that provides guidance to program managers and stakeholders looking to develop SBCC strategies to address malaria medicine issues in their area.
- Cheryl Lettenmaier (Senior Technical Lead, HC3), who will present on the process, findings and lessons learned while conducting the quality malaria medicine campaign in Akwa Ibom, Nigeria.
HC3 encourages professionals working on all ends of the supply chain and health promotion spectrum to register for the event to learn more about how SBCC is being applied to this innovative health topic. There will also be a Springboard follow-up discussion following the webinar for any additional questions or comments.
Please install the The Events Calendar or The Events Calendar Pro Plugin to display a list of upcoming Events






Leave a Reply
Want to join the discussion?Feel free to contribute!